Overview
Ankylosing spondylitis is a chronic inflammatory condition that primarily affects the spine and the sacroiliac joints, which connect the base of the spine to the pelvis. As a form of axial spondyloarthritis, it is characterised by long-term inflammation that can lead to significant pain and stiffness in the back. In advanced stages, this persistent inflammation may cause some of the small bones in the spine to fuse together, resulting in a loss of flexibility and a rigid spinal structure sometimes referred to as “bamboo spine”.
While the condition is most known for its impact on the axial skeleton, it is a systemic disease that can also affect peripheral joints, such as the hips, knees, ankles, and feet. It may also involve the entheses, which are the specific sites where tendons or ligaments attach to the bone.
The onset of this condition typically occurs during late adolescence or early adulthood. While it is more frequently identified in males, females are also affected by the disorder. The progression of the disease varies greatly between individuals; some may experience mild symptoms confined to the lower back, while others may face more extensive involvement of the entire spine and multiple joints.
Causes and Risk Factors
The precise cause of ankylosing spondylitis is not yet fully understood, but it is widely recognised as having a significant hereditary component. Research indicates that the condition is an autoimmune disorder where the body’s immune system incorrectly attacks healthy tissues in the joints and spine.
The most prominent risk factor is a specific genetic variant known as HLA-B27. The majority of individuals with this condition carry this gene, although it is important to note that many people who possess the gene never develop the disease. This suggests that other genetic and environmental triggers likely play a role in activating the condition.
Other medical factors associated with an increased risk include a personal or family history of related inflammatory conditions. These include skin psoriasis, eye inflammation such as uveitis, and inflammatory bowel diseases like Crohn’s disease or ulcerative colitis.
Lifestyle factors can also influence the severity of the condition. Smoking is a significant contributor to poor outcomes, as it has been linked to increased spinal fusion and more severe lung complications in those already affected by the disease.
Symptoms
The symptoms of ankylosing spondylitis typically develop gradually over several months or years. The nature of these symptoms often fluctuates, with periods of worsening inflammation followed by periods of relative stability.
Typical symptoms include:
- Persistent back pain and stiffness: This is usually most severe in the early morning or after long periods of inactivity.
- Improvement with movement: Unlike mechanical back strain, the pain associated with this condition often improves with physical activity and does not get better with rest.
- Fatigue: Many individuals experience extreme tiredness and a general lack of energy, which can interfere with daily activities.
- Peripheral joint pain: Swelling and discomfort may occur in the hips, knees, and ankles.
- Enthesitis: Inflammation at the sites where tendons meet bone can cause significant heel pain or chest wall pain.
Red-flag symptoms requiring urgent medical attention:
- Difficulty breathing: This may occur if the joints between the ribs become inflamed or if the spine begins to curve forward, reducing the capacity of the lungs.
- Eye complications: Redness of the eyes, blurred vision, and increased sensitivity to light can indicate acute eye inflammation.
- Severe immobility: Sudden or progressive difficulty in walking, bending, or turning the head.
Diagnosis
A diagnosis of ankylosing spondylitis involves a comprehensive assessment by a healthcare professional, typically a rheumatologist. Because back pain is a common complaint, a thorough evaluation is necessary to distinguish inflammatory causes from mechanical ones.
Physical Examination The assessment begins with a detailed review of the patient’s medical and family history. A physical examination is conducted to check for range of motion in the spine, chest expansion during breathing, and tenderness in the sacroiliac joints or peripheral limbs.
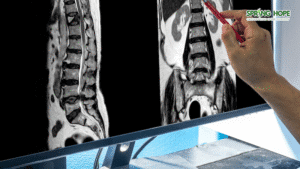
Imaging Tests Imaging is essential for confirming the diagnosis. X-rays of the spine and pelvis are used to look for characteristic changes in the bones and joints. If X-rays are inconclusive but symptoms are suggestive, Magnetic Resonance Imaging (MRI) may be used to detect early signs of inflammation that are not yet visible on an X-ray.
Laboratory Investigations Blood tests may be performed to check for raised inflammatory markers, such as C-reactive protein (CRP) or Erythrocyte Sedimentation Rate (ESR). A blood test for the HLA-B27 gene may also be requested to support the clinical findings.
Treatment Options
While there is currently no cure for ankylosing spondylitis, various treatments are available to manage symptoms, reduce inflammation, and slow the progression of the disease. Treatment plans are tailored to the individual’s specific needs and the severity of their condition.
Medication Categories
- Anti-inflammatory medicines: Non-steroidal anti-inflammatory drugs (NSAIDs) are usually the first line of treatment to relieve pain and stiffness.
- Disease-modifying anti-rheumatic drugs (DMARDs): These may be prescribed to reduce inflammation in peripheral joints like the knees or ankles.
- Biological therapies: For moderate to severe cases, biological agents such as TNF inhibitors or IL-17 inhibitors may be recommended. These target specific proteins in the immune system to stop the inflammatory process.
Physiotherapy and Rehabilitation Physical therapy is a cornerstone of management. A physiotherapist can design a programme focused on stretching, muscle strengthening, and maintaining spinal flexibility. These interventions help to improve posture and maintain lung capacity.
Surgical Treatment Surgery is rarely required but may be considered if there is severe joint damage, particularly in the hips, or if a significant spinal deformity has occurred that impairs function.
Prevention and Lifestyle Management
Management of ankylosing spondylitis relies heavily on maintaining an active lifestyle and making healthy daily choices.
Exercise and Activity Regular physical activity is vital to prevent the spine from becoming stiff in a bent position. Swimming is frequently recommended as it provides a low-impact way to exercise the entire body. Stretching and range-of-motion exercises should be performed daily to maintain mobility.
Posture and Ergonomics Maintaining good posture while sitting, standing, and sleeping is essential. Individuals are encouraged to use supportive mattresses to reduce nighttime discomfort. For those with heel pain, gel-heel cushions in shoes can provide relief during walking.
Smoking Cessation Avoiding smoking is one of the most impactful lifestyle changes a patient can make. Smoking not only worsens spinal inflammation but also compounds breathing difficulties caused by restricted rib cage movement.
When to Seek Medical Attention
Early detection and intervention are key to achieving better long-term outcomes and maintaining quality of life.
It is advisable to consult a healthcare professional if you experience:
- Persistent back pain and stiffness lasting for several months.
- Back pain that is worse after rest or in the early morning.
- A gradual decrease in the flexibility of the spine or neck.
- Pain and swelling in the peripheral joints or heels.
- Redness or pain in the eyes accompanied by light sensitivity.
- Unexplained fatigue or weight loss alongside joint pain.
If symptoms persist or worsen, it is advisable to consult a qualified healthcare professional for proper evaluation.
——————————————————————————–
This page is for general educational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalised assessment and treatment.