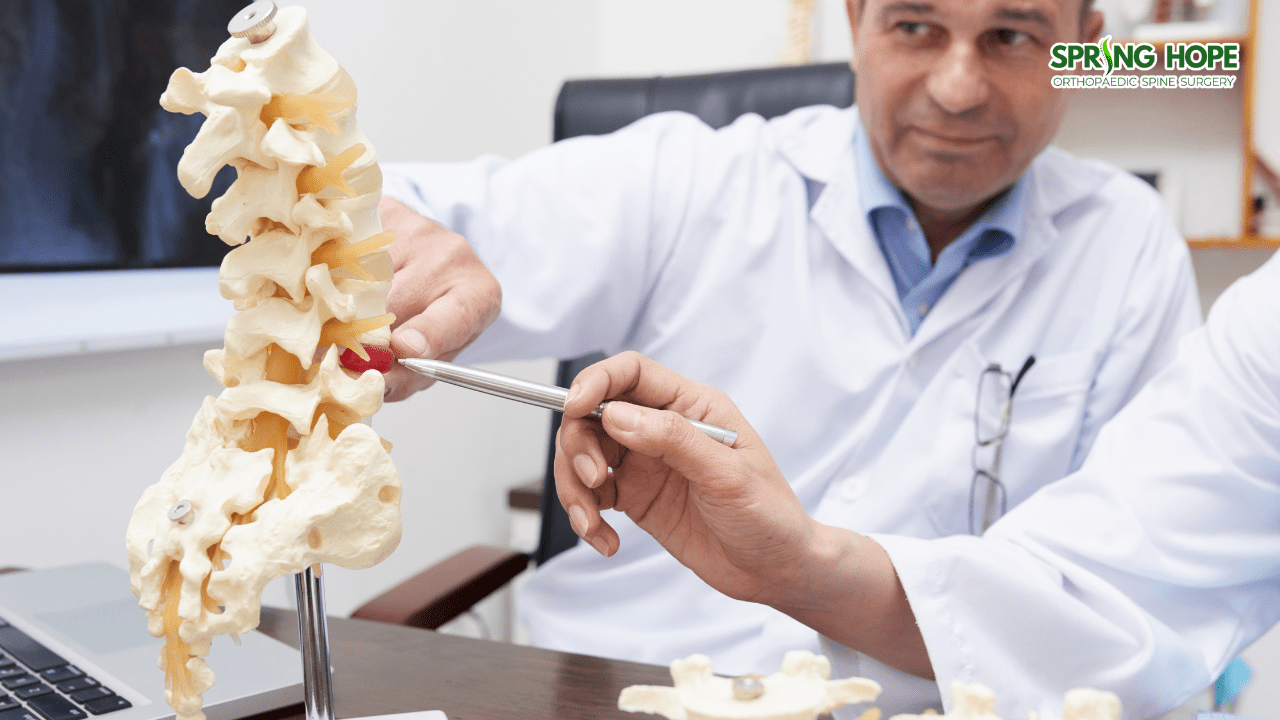
For many individuals struggling with debilitating back or neck pain, the prospect of spine surgery represents a beacon of hope—a chance to reclaim a life free from discomfort and regained mobility. However, the reality of spinal intervention is deeply nuanced. While these procedures are often life-changing, they do not come with absolute guarantees of success.
The spine is an incredibly complex structure, and the path to a successful outcome involves a delicate balance of surgical precision, accurate diagnosis, and patient-specific variables. Understanding why some people find immediate relief while others continue to search for answers is a critical step for anyone considering surgical options.
The Critical Role of an Accurate Diagnosis
Perhaps the most significant factor in determining the success of a spinal procedure is the accuracy of the initial diagnosis. Because the spine is so intricate, symptoms often stem from multiple sources, making it difficult to pinpoint the exact root of the pain or dysfunction.
If a diagnosis is incorrect or even just incomplete, the surgery may fail to address the actual issue. For instance, it is possible for a nerve to be compressed in two different locations. If a surgical plan only addresses one of those areas while leaving the other alone, the patient is likely to experience persistent symptoms after the operation. Without a precise understanding of what is causing the distress, even a technically perfect surgery may not lead to the desired relief.
When Structural Success Meets Biological Limits
It is a common misconception that fixing a structural problem automatically resolves all physical symptoms. In many cases, spinal conditions involve a complex web of nerves, muscles, and bone.
Even when a surgeon successfully corrects a structural abnormality, some factors may not be fully reversible. Chronic nerve damage or long-term muscle weakness can persist long after the physical pressure on the spine has been removed. This means that while the surgery was “successful” from a technical standpoint, the patient’s quality of life may still be affected by these underlying biological issues. Acknowledging these limitations beforehand is essential for maintaining a realistic outlook on recovery.
The Impact of Post-Operative Scar Tissue
Another hurdle in the journey to recovery is the formation of post-operative scar tissue, scientifically known as epidural fibrosis. This tissue can develop around the nerves following surgery, potentially triggering symptoms that feel very similar to those experienced before the procedure.
Interestingly, the way a person’s body forms scar tissue is largely dictated by genetics. This means that some individuals are naturally more prone to developing significant scarring than others, regardless of the surgeon’s skill. Because this factor is biologically driven, it remains one of the more unpredictable variables in spinal surgery outcomes.
How Lifestyle and General Health Influence Recovery
The success of a surgical intervention does not depend solely on what happens in the operating room; the patient’s overall health and lifestyle play a pivotal role in the healing process. Certain factors can significantly impede the body’s ability to recover and integrate the changes made during surgery.
Key lifestyle considerations include:
- Physical Fitness: A lack of physical fitness can slow down the rehabilitation process.
- Smoking and Obesity: Both of these factors are known to hinder healing and can negatively affect the final outcome of the procedure.
- Underlying Conditions: Chronic health issues, such as diabetes or autoimmune diseases, can complicate the post-surgical healing phase.
By addressing these health factors where possible, patients can help maximize their own path to a successful recovery.
Technical Factors and Surgical Strategy
While patient biology is a major factor, the technical execution of the surgery itself is also vital. This includes the specific surgical approach chosen, the techniques employed by the medical team, and the quality of the hardware or implants used.
In some instances, a surgical technique might not fully correct the anatomical problem. In other cases, medical implants may fail to integrate properly with the patient’s natural bone structure. These technical hurdles can lead to complications that prevent the surgery from achieving its intended goal.
Aligning Expectations with Reality
A frequently overlooked reason for dissatisfaction after surgery is a mismatch between what a patient expects and what is realistically achievable. Spine surgery is often about management and improvement rather than a “perfect” fix.
It is vital for patients and their surgical teams to have transparent, detailed discussions regarding the goals of the procedure. By aligning expectations with the most probable results, patients can approach the surgery with a clearer understanding of the potential pitfalls and the promises of the treatment.
Exhausting Conservative Options
Given the complexities and risks associated with spinal surgery, it is often recommended as a final resort. Many spinal conditions can be effectively managed through conservative treatments that do not require invasive intervention.
Before moving toward surgery, patients are typically encouraged to exhaust other avenues, such as:
- Physical Therapy: To strengthen supporting muscles and improve flexibility.
- Pain Management: Utilizing various non-surgical methods to control discomfort.
- Lifestyle Modifications: Adjusting daily habits to reduce strain on the spine.
Key Takeaways for Patients
- Diagnosis is Paramount: Ensure the root cause of the pain is clearly identified before proceeding.
- Biology Matters: Nerve damage and muscle weakness may not be fully reversible even with successful surgery.
- Genetic Factors: Scar tissue formation is genetically controlled and can impact long-term comfort.
- Health Habits: Smoking, obesity, and underlying illnesses like diabetes can complicate recovery.
- Communication is Key: Have honest conversations with your medical provider to align your expectations with realistic outcomes.
Conclusion
Spine surgery remains a powerful tool for improving the lives of those suffering from chronic pain and nerve compression, but it is not a guaranteed cure-all. The journey requires a meticulous approach—starting with a precise diagnosis and a well-considered surgical strategy, and ending with a commitment to a healthy recovery.
For those whom surgery does not provide the hoped-for results, ongoing support and alternative pain management strategies are essential. By staying informed and maintaining realistic expectations, patients can better navigate their options and seek the best possible quality of life.