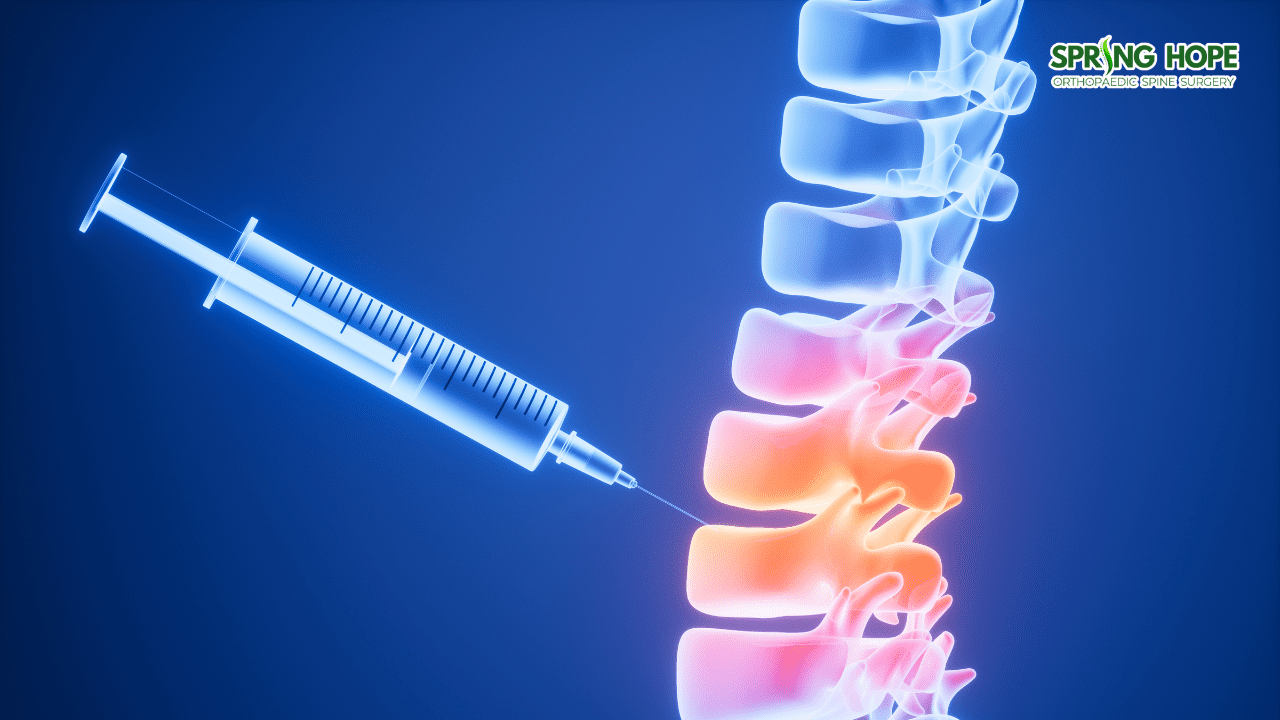
When dealing with persistent back or leg pain, the journey toward relief can often feel like a series of trial-and-error treatments. For many, the transition from initial physical therapy to more advanced interventions is a significant step. One of the most effective tools available in modern spine care is the spinal injection. While the word “injection” might sound routine, these procedures are specialized interventions designed to address the complexities of conditions like spinal stenosis and slipped discs.
Understanding how these injections work, why they are used, and what a patient can expect is essential for anyone navigating spinal health challenges.
Beyond the Standard Clinic Visit: How Spinal Injections Are Performed
It is important to distinguish a spinal injection from the typical vaccinations or blood draws one might receive in a general practitioner’s clinic. Because of the precision required to reach the sensitive areas around the spinal nerves, these are not “ordinary” injections.
To ensure the needle is placed exactly where it needs to be, specialists use X-ray guidance during the procedure. This level of accuracy is vital for both safety and effectiveness. Consequently, these procedures are performed in controlled environments, such as an operating theatre or an interventional radiology suite, rather than a standard exam room. This setup allows for the necessary imaging technology to guide the process, ensuring the treatment is delivered to the specific site of nerve compression.
A Dual Purpose: Diagnosis and Therapy
One of the most interesting aspects of a spinal injection is that it serves two distinct roles: it helps identify the source of pain and provides a window of relief.
The Diagnostic Role
Sometimes, a patient’s symptoms do not perfectly align with what is visible on an MRI scan. For instance, a patient might experience severe pain in their left leg, yet the MRI shows that the nerve compression is actually worse on the right side. In cases where the “clinical picture” and the imaging don’t match, a spinal injection can be used as a diagnostic tool. By targeting a specific nerve, a specialist can confirm whether that particular compression is indeed the source of the patient’s discomfort before considering more invasive options like surgery.
The Therapeutic Role
On the therapeutic side, the injection typically involves a steroid medication delivered directly to the proximity of the compressed nerve. Steroids possess powerful anti-inflammatory properties. By reducing inflammation, the injection suppresses pain signals sent from the spinal nerves, which can lead to improved function in both the lower back and the legs.
When is a Spinal Injection Recommended?
Spinal injections are generally considered a middle-ground treatment. They are often suggested when initial conservative measures—such as oral medications and physical therapy—have not provided sufficient relief.
However, they are also a primary option for patients who are in too much pain to even begin or progress with their physical therapy exercises. By providing a temporary reduction in pain, the injection can “open a door” for the patient to engage more effectively with rehabilitation.
Common conditions treated with this method include:
- Slipped Discs: Where the disc material presses against a nerve.
- Spinal Stenosis: A narrowing of the spaces within the spine that can put pressure on the nerves.
- Specific Disc Issues: In rarer cases, injections may be used for pain stemming from an annular tear or a “leak” in the disc, though these often resolve on their own over time.
The goal of these injections is often to limit or eliminate the need for long-term oral medications and, in some instances, potentially eliminate the need for surgery altogether.
Navigating Safety: When to Exercise Caution
While spinal injections are a valuable tool, they are not suitable for everyone. There are strict contraindications where an injection must not be performed. These include:
- The presence of an infection anywhere in the body, particularly at the injection site.
- Known bleeding disorders.
- The presence of a tumor in the spine.
- Known allergies to the steroid medication, the local anesthetic, or the contrast dye used for X-ray guidance.
Furthermore, there are several medical conditions where a specialist may hesitate or carefully weigh the risks before proceeding. These conditions include uncontrolled diabetes, heart problems such as congestive heart failure, and osteoporosis. Pregnancy is also a major consideration, especially since X-rays are required for the procedure.
Setting Realistic Expectations for Results
It is vital for patients to understand that while spinal injections are often highly effective at relieving back and leg pain, the effects are usually temporary. The duration of relief is variable and can be somewhat unpredictable.
For some, the pain relief may last more than six months—which is considered an excellent result. For others, the relief might last only a few days. Because the recurrence of pain is not always predictable, the injection is often viewed as a way to facilitate further physical therapy. If an injection provides more than six months of relief, a repeat procedure might be recommended in the future if the pain returns.
Key Takeaways
- Specialized Procedure: These injections require X-ray guidance and are performed in sterile, high-tech environments like operating theatres.
- Strategic Diagnosis: They are used to confirm the exact source of pain, especially when MRI results are confusing or contradictory.
- Inflammation Control: The primary mechanism of relief is the anti-inflammatory power of steroids, which quietens pain signals from the nerves.
- Rehabilitation Support: Injections can reduce pain enough to allow patients to successfully complete physical therapy.
- Variable Duration: Relief can last from a few days to over six months, with results over the six-month mark being the ideal outcome.
Conclusion
Spinal injections represent a sophisticated, non-surgical option for managing the debilitating pain associated with nerve compression. By acting as both a diagnostic map and a therapeutic bridge, they allow patients to better understand their condition while gaining the physical relief needed to pursue rehabilitation. While they are not a permanent “cure” and require careful medical screening, they remain a pivotal step for those looking to regain their function and avoid the operating table whenever possible.